Reminiscence of Six Exciting Years as a Surgeon
Base Hospital, Polonnaruwa (1982-1988)

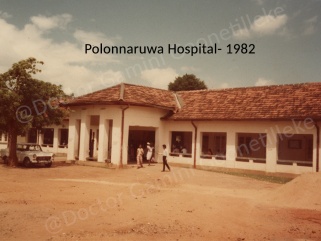
My first posting
I was 32 years old, just returned after qualifying as a Fellow of the Royal College of Surgeons (FRCS) and a post graduate training in the UK. After a short spell as the Resident Surgeon of the Accident Service of the General Hospital Colombo, I asked for a transfer from this unit. I was offered the post of Consultant Surgeon at the Base Hospital, Polonnaruwa.
I was in two minds. I had never worked out of Colombo and I was warned that Polonnaruwa was infested with Malaria. Moreover, there was also the danger of being exposed to wild elephants. Some even said that this might be considered a punishment transfer. It was only the encouragement given by my friend, batch mate and colleague, the late Dr B F S Samaranayake (Sam) who was the District Medical Officer (DMO) at Base Hospital, Polonnaruwa that made me finally take the plunge.
I had no idea what my future would be. One thing however, I was sure. The people and their welfare would be uppermost in my mind.


Background
- There were three hospitals in the District of Polonnaruwa.
- The main hospital in Polonnaruwa was equipped with surgical facilities and a surgeon was appointed at the end of the 1970’s
- Three specialists were appointed – Surgeon / Physician / Obstetrician & Gynaecologist. Surprisingly an anaesthetist was not appointed to the hospital.
- Population served was 260,000
- The nearest hospital to Polonnaruwa with surgical facilities was 115 Km away in case a patient had to be transferred.
Move to Polonnaruwa – Initial Problems – Living Facilities & Other Issues
- My first journey to Polonnaruwa to accept the job was by train and it took 7 long hours to travel 240Km.
- I lived in a room in an old dilapidated building adjoining the hospital. The facilities within the room were less than basic. There was no choice. I spent six months in this room until the official Surgeon’s quarters were repaired and renovated.
- Travel to Colombo once in two months or so, was by bus or train and that took six to eight hours.
- My salary was Rs 2200/= per month. I was entitled to private practice, but there was no Nursing Home to perform surgery. It was only a Consultation practice, the fee per patient being Rs 25/=


Visit to the Hospital / Hospital Facilities
- There were more patients than the number of beds. The waiting list was long as there was no surgeon for a while.
- There were no junior Medical Officers in the ward. The House Officers were Registered Medical Practitioners (RMP).
- There was a small lab which could only do two investigations, namely urine, full report and full blood counts. The Blood Bank was primitive and so was the Radiology section. Only Plain X ray’s could be done.
- The Operating Theatre had an old operating table, a dim light and an old Boyle’s anesthetic machine.
- However, the nursing and other staff members were very enthusiastic, keen to work and promised to extend their cooperation.
Starting Work
- I started work and performed ward rounds and held clinics daily.
- Surgery was also started on a low key on a daily basis under local anaesthesia.
- I was on call in the surgical wards 24/7.
- Whatever I could not manage was transferred by ambulance to hospitals at Matale and Kandy many Km away.

In the absence of proper facilities for investigations, I had to practice what every budding doctor learns In Medical College – take a good history and examine the patient well. That will give a correct diagnosis on most occasions. It also reminded me of Lord Platt who said: “if you listen to your patient long enough, he/she would tell you what is wrong, thus demonstrating the value of what is called bedside medicine”.
Equipment
I obtained the equipment necessary for my work from the Health Department stores in Colombo. They officers there were more than happy to help to supply the equipment to do my job efficiently.
Learning Anesthesia
Some patients needed to be anaesthetised for surgery. There was no Anaesthetist and I was not competent to do that job. So I decided to follow a crash course in anaesthesia with a Consultant Anaesthetist in Colombo for two weeks. I learnt regional blocks, spinal anaesthesia, tracheal intubation and some aspects of general anaesthesia which would suffice for my work. I started operating after anaesthetising my patients when necessary. Intravenous Thiopentone was used to induce anaesthesia which was maintained with Halothane, oxygen and nitrous oxide for the duration of the surgery. It was indeed a risk, but risks had to be taken. I collected the data on my experience in this field and submitted a paper for the Annual Sessions of The College of Anaesthesiologists. The title of the paper was “The Role of a Surgeon as an Anaesthetist”. The President of that Association said that “a surgeon has no role as an anaesthethist”. That first academic paper that I submitted to a medical association was rejected and ended in the dust bin of history. But I did not give up. More academic papers were to follow.
Junior Medical Officers

There was a dire need for junior medical officers in the hospital. Sri Lankan doctors were reluctant to work at the Polonnaruwa Hospital for various reasons. The Department of Health finally had to appeal to the World Health Organisation (WHO) to get down overseas doctors to fill the gap. They selected doctors from Burma for a period of two years and sent them to the Polonnaruwa Hospital. There was an Anesthetist as well in the Burmese team. This suited me well although they did not understand Sinhala.
Recognition by the Sri Lanka Medical Council
The Sri Lanka Medical Council decided to recognize the Polonnaruwa base Hospital for training of Intern Medical Officers in view of the wide variety of clinical conditions being treated by the specialists in the hospital. This cleared the way for local doctors to be appointed to the hospital for their internship training. An anaesthethist too was appointed after the departure of the Burmese doctors.
Improving the Operating Theatre:
The operating theatre too was modernized with new equipment being supplied by the Japan International Cooperation agency (JICA). They were helping rural hospitals and my request to JICA was accepted. This made a huge difference to the hospital and I was able to serve the people better.


Surgical Problems
The Surgical problems encountered were vast and varied – hernias, goitres, cancers of various organs, kidney stones, abdominal emergencies, injuries caused by trap guns, by wild animals such as bear, wild buffalo and elephants, by agricultural machinery, stabs, assaults, burns and those caused by road accidents. Half of the workload was related to trauma. The management of the surgical patients will be described in the subsequent posts.
Transformation of Hospital
- Improvement of facilities with increase in the bed strength
- The recognition of the hospital by the Sri Lanka Medical Council for training of Intern medical officers was a significant change.
- An upper gastro-intestinal Endoscopy Unit, too, was set up with support from JICA.
- The setting up of a special military ward and the management of war casualties added extra impetus to this hospital.
- Opening of a small Intensive care unit with two beds
- Inaugurate a Clinical Society for the District for medical interaction and fellowship
- The presentation of scientific papers, publications and orations from data collected at this hospital brought recognition not only to the Consultants, but to the hospital as well.

MANY ORGANISATIONS VOLUNTEERED TO IMPROVE THE HOSPITAL



Departure from Polonnaruwa
After working for over six years, the time had come for me to leave Polonnaruwa. It was heart-breaking to say the least. This was a period where I had to work in relative professional isolation. The scope of practice was wide with limited resources to get the job done. The period was highly rewarding in terms of the lessons learnt although under high pressure at times.
Photos with staff and patients prior to my departure from Polonnaruwa

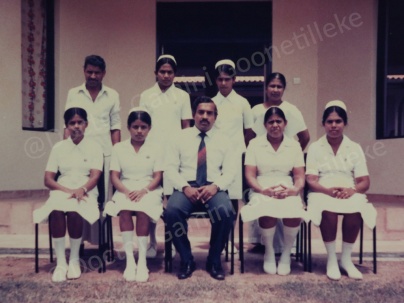
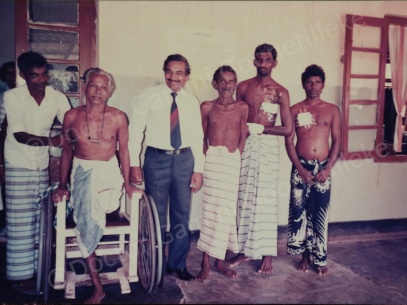

As a General Surgeon in a rural hospital with limited resources, I had to perform surgery on many patients suffering from a wide variety of surgical diseases and injuries incorporating almost all branches of surgical specialization. This was truly a learning experience or what is called today “Experiential Learning”

“A challenge awaits us with each new day breaking.
Run swiftly to it, it’s yours for the taking”
Video Links:
Keywords : Polonnaruwa, rural surgery, farming injuries, surgical challenges, injuries, surgical innovation, war injuries, land mines, antipersonnel mines, general surgery, saving life, surgical education.
Dear Reader, if you like to read more about my web stories, you might want to read my next story, where I get my first exposure to war injuries : FIRST EXPOSURE TO WAR INJURIES
Please feel free to share story this with your friends :
47 thoughts on “Reminiscence of Six Exciting Years as a Surgeon”
A great capacity to adapt to the circumstances and serve the people
I saw the conditions in 1991 and I believe in what I saw.
You’ve gone beyond the call of duty of a surgeon
Interesting article showing your commitment to society
Very interesting to read what a lot of dedication two lessons to learn 1) Talking to patients for a long time to diagnose 2) If the commitment is there everything is possible even with the least equipments available your efforts to learn to be a competent anesthetic is greatly admired the Dictors of today gave much to learn from people like you we are proud Dr Gamini
Dear Joe
Thanks for your comment. Much appreciated. I hope you will enjoy reading the other stories as well.
Best wishes
Gamini
Sorry error :”Doctors Doctors of today have much to learn
Very interesting reading.Sir,you are a doctor to be admired for going beyond the call of duty.
Dear sir,
Dedication ,determination ,skills,
Those are the key ingredients I experienced working wirh you.
What wonderful journey down the memory lane. Love to share the article. Good luck with your future endures.
Thank you for your wonderful service to humanity
An exciting medical career with many ups and downs and your service to the nation is deeply appreciated
Proud of you
Surgeon par excellence
An exciting story and an exceptional life! Stay blessed
With an FRCS in the bag, selfless service to the poor with limited resources & in professional isolation has brought out the best in you.
Those blessing of the poor accumiliated turned you out to be a blessed human being that you are today.
That experience & your determination surpass that FRCS & has placed you on a higher pedestal by the poor humble Countrymen.
Thank you & may many be fortunate to be treated by the hands of this blessed Surgeon.
Doctor I worked as a rural school teacher in a small village in Uwa around those years and we didn’t have even basic materials coloured chalk which I bought from Gunaseas before taking the Udarata Manike from Fort. As such and having experienced such rural conditions , I can imagine under what conditios you had to work as a surgeon often in critical situations of life and death. I can well imagine what you meant to those.poor people as you went about easing pain and saving.lives. The reward of fond memories will inspire young doctors and also underline the simple theory that if you care you can overcome difficulties and definitely make a difference. Bless your healing hands and caring heart..
I was the Regional Director of health services during a short period of the tenure of Dr.Gamini Gunatilaka as the first surgeon at Polonnaruwa hospital. Although I had not met him then I am aware that he dedicated himself to the establishment of the surgical unit there. He had versatile qualities which made him very popular with the staff and the public.
In the absence of specialized investigations, you had the habit of ‘patiently’ listening to patients to find out details of the illness – “Bedside Medicine”
Two more gifted ingredients that you possess are your Pleasant smile and Appetite to give the best to the patients.
You have done your part Well for the Well being of the human kind.
You are a Blessed creation of Almighty God that we both trust and believe.
Devoted Surgeons like you are rear to find God Blessing
I enjoyed reading this just like the way your book ”In the Line of Duty – Life and Times of a Surgeon in War and Peace”
Those were the days.
carry on my friends !!
WOW. What a blessed and a colourful life. Praise God for all his goodness and protection.
Great stuff Gamini. Every episode makes my admiration of you grow more and more.
Take care & God Bless
An extraordinary experience under exceptional and challenging circumstances
You still look groovy!
Behind all that maturity you cant hide the naughtiness!
Take care and keep doing all your good work.
It is very inspiring, very courageous and with awesome risks.
Can’t even imagine the experience and the lessons learnt! I don’t think as eloquent as you are, can express in words or slides those six years. One of the most amazing things is the enthusiasm of the staff.
Doctors of your caliber are a rare commodity in Sri Lanka these days. God will truly bless you for the exceptional surgeon you were, and for your dedication not only towards your patients but towards the “have nots” of the society you served
This story enables me to go back into my past, when I first met you at Polonnaruwa. I remember those halcyon days with a lot of pleasure.
This is a story of a true hero who displayed courage and dedication to serving the common folks in a remote town far away from the city where he was used to enjoying all the comforts that life could give. Very proud to know and be related to such a humble and selfless person!!. if only SL had more leaders like Gamini who put the cause before personal benefit, it would be a better country for all.
Most of today’s Medical Fraternity use their knowledge to just make money. This results in
Patients being treated as geese that lay the golden egg and on the flip side there is nothing
creative evolving from all the knowledge they have gleaned through all the education
they have obtained. Probably that’s why there are more sick and more pandemics
these days.
“ Experiential Learning” and less facilities may bring on the vital holistic dimensions of
overall healing.
Doctor your life experience should be included in the syllabus of all aspiring Medics.
What an inspiring story of medical leadership.
Absolutely great Dr. Gamini .
Dear sir
Im so glad that i learnt ABCs of surgery from you and to start my carrier as an intern with you.
Wish you all the very best
Thank you very much Sir.
We always had the highest admiration for you Gamini
The story is superbly written
God Bless
Nihal
Great my friend
Dear Sir,
I belive that every job is a Self-Portrait of the person who did it. So, everyone can see your determination and strength you had developed to face challenges in your professional career. You had great enthusiasm what you were doing . You have no debt to pay back to the country and you had done enough. God blessings with you forever Sir…I wish you good health and a long life
Wonderful motivation for up and coming doctors
As a former student of St Josephs College, Colombo I am proud of Dr. Gamini Gonnetilleke’s achievements and service to humanity.
Every good wish
Your commitment to your profession is abundantly clear.
Take a bow!
Dear Gamini
The best compliment I could pay you is that the present and future generation of doctors should try to emulate you.
There no words to express what a great man you are what a great heart you have. I enjoy every article you write with pleasure and pride. You truly are a pride for St Joseph’s. You are a great example for doctors of today as well, as most of them do not have the dedication that you have, I consider some of them as just Mudalalis!!!
There no words to express what a great man you are what a great heart you have. I enjoy every article you write with pleasure and pride. You are a great example for doctors of today as well, as most of them do not have the dedication that you have, I consider some of them as just Mudalalis!!!
Thank you for your dedicated services and the unfailing strength and optimism with which you improved the medical conditions for the people of Polnnaruwa. It should be every doctor’s mission and will serve the patients.
I am privileged to know you personally Dr. Gamini. I have always had a great admiration of the work you do for the poor people especially. More than money your love, commitment and dedication are sometimes forgotten by many present day doctors. As you yourself has told me so many times, you always put the interest and welfare of the patient before your own personal interest or comfort. You have always shown that being a doctor is a VOCATION and not a Job. I have spoken about you to many a young doctor and especially to many young men and women who are aspiring to be doctors. I would very much like to introduce some of these young medics to you. Just talking to you and listening to your many experiences and exploits will itself be a great learning experience for them. Many of what you have done will not be found in medical books. Your experience is a gold mine for all future doctors and also for those who think that nothing can be done in the present situation. If there is a will and a way, Miracles take place when challenges are turned into opportunities. You are a shining example. So proud of you. Love you always.
This is the real book shares his experience to us lively and thanks for your dedicated service to motherland. Good luck for your future endeavors.
Dr Gamini was my classmate for 7 years and at AL we were seated together at St Joseph’s College, Col 10. Gamini was the best in our AL class for dissections of frogs, rats, earth worms, small sharks. I was the worse. I told Gamini several times that he will be a good surgeon. I knew the word surgeon from my Mother who was a nurse. Gamini had the talent skill and patients to dissect at AL class. He won the Class Prize in Zoology. Dr Gamini brings honor and Pride to St Joseph’s and our Class of 1949. 10 of us meet daily thru WhatsApp exchanging videos, chats. May God bless this dedicated Surgeon. My Class of 1949 produced Niranjan Devaditiye, MP of the House of Commons during Magaret Thatchers time and later a MP of the European Union representing South London. We have the culture from our family background and St Joseph’s. Gaminis dedication comes from these 2 culture institutions. What a Class of 1949.
Sunil Lasantha Perera